Hello, and welcome back. Today we are talking about your plantar fascia and all things plantar fasciitis:
- How do you know if you have plantar fasciitis?
- What Is Plantar Fasciitis
- What Causes Plantar Fasciitis
- Will Plantar Fasciitis Heal on it’s own?
- What to do if it doesn’t heal?
- How To Avoid Surgery for Plantar Fasciitis?
Plantar fasciitis is one of the most common things we see especially with a lot of our hikers. Since we have such good weather all year round. We have a lot of snowbirds that come here in the winters and we have people who make it a point to hike all the Arizona trails as much as they can at least nine or 10 months out of the year. So plantar fasciitis is in abundance when it comes to one of the top things that give people trouble here in the Valley.
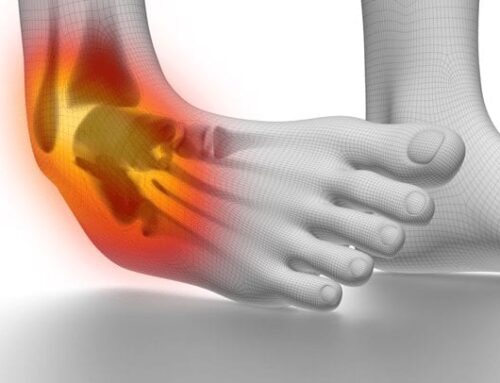
How do you know if you have plantar fasciitis?
Usually this is characterized by heel pain at the base of your heels, so where the front of your heel is rather than the back of your heel, and it’s usually the most painful first steps in the morning. And then it’ll get better as you walk around throughout the day. But you’ll find that if you sit in one place for a long period of time, and then stand up and start walking around again, it’ll hurt just as badly as it had before.
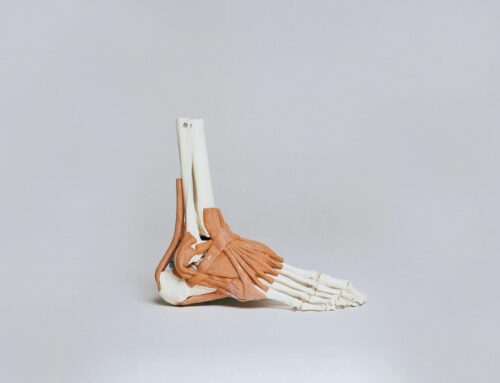
Now the reason for this is pretty simple. The plantar fascia is this band of thick tissue that runs across the bottom of your foot. And its main job is to support the arch of your foot. So really, if you take your foot and pull your big toe back, what you should feel on the bottom of your foot if you’re touching the bottom of your foot with your other hand or you can even see it with your eyes is a thick band of tissue rise against the skin on the bottom of your foot. This is your plantar fascia.
When your big toe goes back during normal walking or running patterns, that fascia is supposed to get really taught to give the arch a lot of rigidity or structure & make it a lot more stable. When that big toe gets pulled back. It causes strain in that plantar fascia. Oftentimes, whenever you do pull the big toe back, people with really severe plantar fascia will feel that in the area that they have plantar fasciitis. The reason that it starts hurting whenever you get up and you start walking around again, is because whenever you’re in a relaxed position, let’s say at night, when you’re sleeping and your feet are pointed down, or just in a relaxed position, the plantar fascia begins to heal. Then in the morning, when you go to get up, it causes re-tearing of whatever has healed. So you’re just kind of stuck in the state as if you had a paper cut, and it was healing overnight. And then you went and you pulled that paper cut open each morning, you’re basically starting with a fresh new injury.
What Causes Plantar Fascia Pain?
There are several reasons that the plantar fascia gets so irritated to begin with, but ultimately, this is what’s known as a degenerative condition. What that means is that it doesn’t happen in one big fell swoop or injury. But it happens over time. So by the time that individuals start experiencing any sort of heel pain, they’ve actually had degeneration in their plantar fascia for a much longer period of time. Usually, the reason for this is because of some sort of altered mechanics or load sharing between the hip, knee and ankle, and the arch is excessively collapsing over a long period of time.
Now, another cause of it could be calf tightness. So basically what happens during normal walking, if your calves are tight, or your hips are weak, you will have a collapse of your arch. This is called pronation. And a lot of people have heard about pronation, and for a long time, it’s been made out to be like the devil’s motion, because it can cause so much injury at your foot, knee, or hip, and it can even cause altered shock absorption, which causes back issues over a long period of time. The thing about pronation is that it’s been over demonized, and your body actually needs some amount of pronation in order to absorb shock and force during normal walking or during running.
The reason that I bring this up is because a lot of people have been sold into anti pronation shoes or really rigid orthotics that don’t allow for any pronation because pronation should be avoided at all costs, when the truth is that if you have footwear or foot support that is too rigid, it’s actually going to cause other issues up the chain whether that’s going to be in your knee or hip or back, because the arch doesn’t give at all. What’s important to know is that you do need some pronation, but excessive pronation caused by either weak ankle and foot muscles, tight calves, or weak hip muscles is what ultimately causes excessive pronation again and again over the day, which stretches the plantar fascia again and again and again, ultimately leading to degeneration and leading to what we know as plantar fasciitis.
Anybody can get plantar fasciitis. It can be a young athlete, it can be an older individual, it can be a lot of those hikers that I talked about, it can be people who walk golf courses, or anybody who’s generally more active, or people who are a little bit more sedentary that have put on a little bit of weight over the past few years, and haven’t kept up with strengthening or cardiovascular activity, the arch is not prepared to accept the increase in load and over time you will still experience that degeneration.
Will Plantar Fascia Pain Go Away On It’s Own?
One question that a lot of people have is will plantar fasciitis just heal on its own or go away? The answer is that it might get better for a little while if you take enough NSAIDs or anti-inflammatory medication and you ice it, and you stretch your calves and things like that. But if you don’t figure out why it happened in the first place, for example, if it is hip weakness, which is caused by a pelvic rotation, or if it is that your muscles in your foot and ankle don’t have the appropriate stability and control or you’re lacking joint mobility in your ankles, so it causes your arch to collapse… If you don’t fix the primary reason that it’s happening in the first place, then even though it goes away for a little while, what a lot of people struggle with is that it rears its head and comes back again later on.
The other thing to consider is that there are other things that can seem like plantar fasciitis. The easiest example here is that it can be a nerve entrapment in the plantar fascia in the bottom of your foot. There are nerves, one of them being the calcaneal nerve that can become entrapped, meaning just that stuck in other tissues. The nerve can give off very similar pain representation that would be similar for plantar fasciitis.
I have this client who came in who had plantar fasciitis for eight months, and she had been in a boot for six months. This is one of the more common treatments that we’ve seen for plantar fasciitis that really never works out is putting people in a boot because it causes so much atrophy and muscle loss and different movement patterns that these people end up with more issues than they started with. But by the time that she got the boot removed, her plantar fascia had largely healed, but she had very, very similar pain patterns. And what ended up being revealed was that it was nerve entrapment in the arch of her foot where the plantar fascia when it had been inflamed as it went through his healing process had likely just healed over the nerve a little bit and was tugging on the nerve as she would take steps.
Once we released that it was in very short order that she was restored to normal walking and had no further issues. But then we had to go through all the strengthening cycles and processes to undo what putting her in a boot had been prescribed for in the first place.
Another reason that people have been told that they have plantar fasciitis is heel spurs. When it comes to heel spurs, what that means is that there has been a calcification or an extra growth of bone along the heel bone, which is called your calcaneus. They’re theorizing that that spur is tearing the plantar fascia. Now the problem with this is that a lot of people have heel spurs and never develop plantar fasciitis. The only case in which I could see this actually being a possibility is if that heel spur is pushing into the plantar fascia as a result of the arch collapsing. When the arch collapses, it’s getting a double insult, it’s getting stretched, which is that over pronation that we talked about constantly pulling at it, in addition to that spur being thrust into it. Now if that’s the case, then yes, absolutely the heel spur can be a contributing factor. However, a lot of people sell it as when they do an image and they see a heel spur, they say that’s the only thing that’s causing someone’s plantar fasciitis. Then when that person goes through surgery to get the heel spur removed, often they’re disappointed to find that the plantar fasciitis still comes back up years or months later.
What are the Best Treatments for the Plantar Fascia?
Options:
- NSAIDS
- Orthotics
- Boot
- Crutches
- Injections
- Surgery
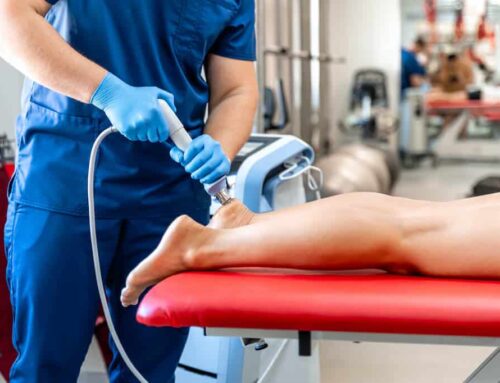
Now let’s talk about best treatments and treatments to avoid for plantar fasciitis. Treatments that might be prescribed to address inflammation are anywhere from non steroidal anti inflammatories like Advil, Aleve, or Ibuprofen, or something stronger.
You might be prescribed orthotics, a walking boot, cane or crutches. These are all ways to unload the plantar fascia, but we’ve already talked about why those will only relieve the symptoms and reduce the inflammation, and all those mechanical things will still exist, which will cause the degeneration just to bring it right back later on.
Some of the more invasive options are injections. They might recommend injecting a steroid medication into the area. But the limiting factor here is that you can’t do a whole lot of these because the nature of these injections is that they also weaken the plantar fascia. So over time, even though these medications rapidly reduce the inflammation, they also increase the likelihood that you will have this issue in the future.
Surgery is very rarely done, but in severe cases that have been non responsive. And oftentimes, these are the cases that have just been mismanaged for long enough and then haven’t been treated appropriately in the first place, they will offer a surgery to detach the plantar fascia from the heel bone. This will just serve to destabilize your foot, you’ll no longer have what’s called the Windlass mechanism, which is what I spoke about earlier, when you pull the big toe back, the plantar fascia gets rigid to provide support for the arch. What will happen instead is since that’s not there, your foot will be more prone to collapsing, which over time will cause increased muscle and tendon issue and strain and also cause a variety of force absorption issues which could cause further issues in your knee and the hip.
Surgery absolutely should be avoided at all costs. And the best way to do that is making sure that you get it treated correctly in the first place. A couple of the newer therapies we’ll discuss here, there’s something called shockwave therapy, which actually has been shown to have great benefits lately, which will send basically soundwaves into the area to break up scar tissue and stimulate healing. And again, this will have great effect on the tissue but again won’t correct those biomechanical issues that cause it in the first place. So these types of therapies are best used in conjunction with therapies that are directed at finding out the real cause for having the plantar fasciitis in the first place, that root cause.
The other type of injection is regenerative medicine. It is injected into the area of the issue, which will stimulate a rapid healing response, which has been proven and is showing to generate really great results very similar to shockwave therapy. Again, you’re limited by not having restored the actual mechanics, whether it’s a hip weakness or whether it’s joint immobility or anything else that might be causing you to have plantar fasciitis in the first place.
When it comes down to it, there is no best treatment method for plantar fasciitis because it is dependent on the individual. Let’s say that you’re an individual who has had chronic ankle sprains. Well, when you have chronic ankle sprains your ankle is looser by nature because you’ve sprained the ligaments time and time again. One of the things that your body does to protect against that is tighten up your calf muscles. When your calf muscles tighten up, because they’re guarding and trying to stabilize the area that may cause over pronation, which again, will then lead to plantar fasciitis. Another type of individual might have any sort of hip or pelvic or back injury that leads to impaired hip mechanics or just the inability to absorb shock and altered ways of moving that cause them to pronate during their walking cycle, which will eventually cause that plantar fasciitis to rear up.
In both of these cases, in the chronic ankle sprain case, and in the person with a hip or pelvic or back issue case, you’ve got to solve that in order to create a long lasting solution to the plantar fasciitis. Not only do you need to do the things that are going to relieve the pain, like stretch the calf muscles and mobilize the ankle joint and perhaps use a golf ball on the plantar fascia, or ice to just take the edge off the pain even though that’s not going to be what’s best for long term healing…You need to combine that stuff with the corrective things for the tight calves and the weak hips and everything like that.
Orthotics is another thing that we touched on, in my opinion, they can be used as a treatment method. It’s something that you should use for now, but not forever, as long as you still have a good arch. If you used to have an arch and your arch has absolutely collapsed and you no longer have any sort of arch anymore, even when you pick your foot up off the ground, that’s one scenario in which you might need orthotics that are more permanent. But if when you pick your foot up off the ground and goes from flat to actually having an arch, then that means there might be something that could be done from a muscular perspective, from a joint mobilization perspective, to get your body to use that arch more appropriately again.
I think that orthotics can be used in a temporary solution to cause less pronation, not absolute stop of pronation but a little bit less pronation when you’re walking to allow that plantar fascia that time to heal, but should not be used over a longer period of time, or indefinitely. When you support the arch over a long period of time with orthotics indefinitely, then what’s going to happen is naturally the muscles that should be doing that are going to get lazy or stay lazy and not do their jobs. And so you’re going to still have weak arches over a long period of time, which is going to cause this issue to just come back again and again.
The idea is to make it go away, not just for now, but forever. So if you’ve got plantar fasciitis or know someone who’s got plantar fasciitis and you’re struggling to know whether it’s actually what you have because everything that you try seems to only give short term results, make sure you get it accurately diagnosed by a doctor of physical therapy.
There is not a lot of imaging that goes along with this, again, as a lot of symptom based type things is enough to diagnose plantar fasciitis is it’s those first steps in the morning, it’s the location of the pain, and it’s the absence of other reasons that would cause that pain.
So make sure that whoever you’re working with is going to help you understand the reasons that it happened in the first place, whether that is decreased hip strength, improper pelvic position, decreased foot and Ankle strength, or whatever it might be. That way you can design a long lasting solution because the last thing you want is for this issue to keep coming back again and again until surgical intervention or long term orthotics or canes or anything like that is something that is an absolute necessity.
If you would like to know more about how to work with one of our experts from anywhere in the US, be sure to fill out a contact form requesting more information.