In our previous post we discussed how the balance system works, defined Benign Paroxysmal Positional Vertigo (BPPV or vertigo for short), and went into the basics of the anatomy that makes up the vestibular system. Today we will go into how to tell if your dizziness is caused by BPPV and how to treat it if it is actually vertigo.

giphy.com
Step 1: direct classic film noir movie
There are a few signs and symptoms of BPPV that set it apart from other balance disorders and make a proper diagnosis easier. These include:
-
Short bouts of dizziness (usually <1 minute; NOT constant dizziness)
-
Triggered by movement in a certain direction or a change in position (ex: rolling in bed to the left, looking over the right shoulder, etc)
-
Abnormal rhythmic eye movements (nystagmus) during vertigo attacks
 giphy.com
giphy.com
Nystagmus
BPPV does not directly involve irritation of any nerves or blood vessels, so there are no neurological issues with this condition. If there are signs of hearing changes, headaches, numbness, trouble speaking, or loss of consciousness that accompany the episodes of dizziness, then there is likely something else going on that needs immediate attention.
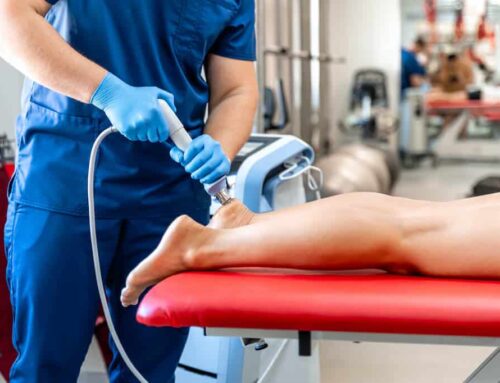
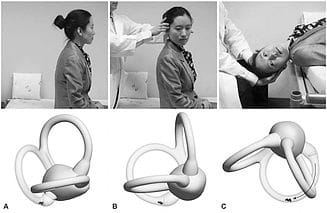
Since BPPV is caused by crystals moving out of place in the inner ear, testing for vertigo involves recreating this motion to see if the symptoms come on. After talking with your healthcare provider to determine if BPPV is a real possibility, a simple test called the Dix-Hallpike can be performed in-house. The patient sits on a treatment table with the physical therapist (PT) holding their head turned slightly to one side. In a quick, continuous motion the the patient lies back as the PT supports the head in the rotated position. The patient keeps their eyes open for the PT to check for nystagmus and also reports if they are feeling their vertigo symptoms. If the test does not produce any results, then it is repeated with the head turned to the other side.
researchgate.net
The Dix-Hallpike Procedure
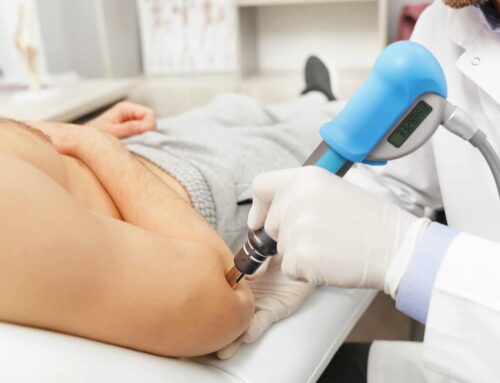
If there is a positive result for the Dix-Halpike procedure, then treatment can be performed immediately afterwards via the Epley Maneuver. The procedure begins just like the Dix-Hallpike: the patient sits on the treatment table with their head turned to one side and the PT quickly guides the patient down while keeping their head in the correct position. The eyes are kept open to check for nystagmus and the patient informs the PT of any symptoms being felt. The position is held until the patient’s symptoms have passed. The patient and PT stay in this first position for an additional 30-60 seconds to allow all of the rogue crystals in the inner ear to settle into their new position. Next the PT quickly turns the head to the opposite side without the patient moving their body. The eyes are kept open and the patient continues to update the PT on their status. Another 30-60 seconds passes, then the therapist has the patient roll onto their side while keeping the head in the same position. This puts the patient on their with the head pointed towards the ground. Another 30-60 seconds pass to let the crystals settle in the inner ear and then the patient sits up while the PT maintains their head in the neutral position.
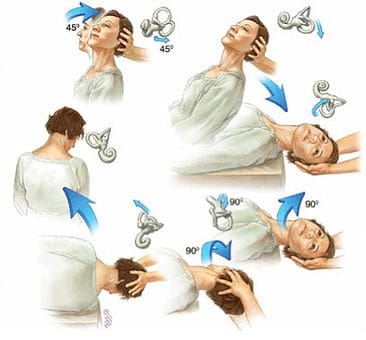
The Ashgrove Spinal Centre
The Epley Maneuver
Good News & Bad News Time: The good news is that significant relief of symptoms usually come withing minutes or hours of treatment. It is normal to feel some residual dizziness in the hours following the Epley Maneuver, but relief can be long-lasting afterwards. In many cases 1-2 sessions is all that is needed to get complete (or nearly complete) relief of BPPV symptoms. The bad news is that BPPV has a high rate of recurrence. Up to 50% of people will experience symptoms again within 5 years. If it always seems to occur in the same way, it may be beneficial for the PT to teach the patient how to self-treat so that the problem can be addressed earlier.
The examples of tests and treatment given today are for the most common location and type of BPPV, posterior canalithiasis. There are other procedures that are used for the different types and locations of BPPV, so having a proper diagnosis from a healthcare provider is essential before starting any treatments at home. For more information, visit the Vestibular Disorders Association website.