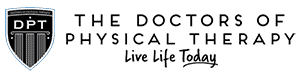What causes plantar fasciitis?
Plantar fasciitis typically develops over time as the plantar fascia undergoes small injuries day after day until eventually the level of injury gets to a point that it causes pain. These injuries may occur whether you are an active runner (see our blog on plantar fasciitis and running) or you are relatively sedentary.
If you do not regularly participate in physical activity it may seem strange to you that your foot has suddenly become injured. Some of the contributing factors in this case may include: improper footwear, tight calf musculature, or general lower body weakness. If you stand for long periods of time, improper footwear includes sandals, flats, or flip-flops without arch support. This lack of arch support over a long period of time places increased demand on both the plantar fascia and the musculature, bones, and ligaments that support the arch of your foot, eventually leading to damage to the muscle, the plantar fascia, or both. Tight calf musculature may force you to walk differently, with your toes pointed slightly outward instead of forward. This position allows you to roll off of the inside of your foot instead of over the ball of your foot. While this keeps you progressing at your normal rate, it places increased load through the arch and allows your arch to collapse. This occurs commonly with people who are required to work at a desk or wear heels for most of the day. Weakness of your ankle musculature, particularly the muscles that support the arch can also contribute to the development of plantar fasciitis. This can happen if you do not regularly participate in physical activity.
This list of causes is not comprehensive, as there are other causes of plantar fasciitis such as weakness of the hips and other postural muscles. This is why it is important that if you have plantar fasciitis, to consult your doctor of physical therapy to determine the contributing factors, and how to best prevent it from coming back.
So how do you avoid making it worse? The worst thing to do with plantar fasciitis is wait to get it addressed and only managing the symptoms. Without addressing the root causes of the condition it is almost certain that it will get worse or come back. In the meantime you need to unload the plantar fascia. Do this by wearing shoes with good arch support or getting some orthotic inserts. I typically recommend superfeet and provide my patients with a specific model based on my evaluation. If you can comfortably sleep with a night splint you may do so, but in many cases this may be overly aggressive. If you wear high heels during the day, you should start progressing yourself to lower heels, and if you can get rid of them completely for a while without increasing the pain, do so.
http://1.bp.blogspot.com
What are the best treatment options? This ties in well with how to not make it worse. Until it is healed you need to wear supportive shoes. To help it feel better, you can roll your foot over a frozen water bottle for five minutes a couple of times a day. Getting out of pain and managing the symptoms is just the first step. In order to fully heal your plantar fasciitis and make sure it doesn’t come back you need to address the cause. If the cause is tight calf musculature, you may start using a foam roller or getting a massage to relieve the tightness in the calves. This may be supplemented with a calf stretch. If the cause is weakness, you need to strengthen the select muscle groups. Many of these causes cannot be determined without a movement analysis and evaluation. With this data, your physical therapist will be able to assess the causes and provide you with guidance through the healing process. They may use a variety of techniques including taping, modalities, manual techniques, and exercise prescription to facilitate your recovery. As with any injury, the best form of treatment is prevention. To prevent this from happening to you, make sure you maintain a good strength and flexibility program for your legs with the following exercises.
-
Calf stretch with knee straight and bent.
-
Heel raises
-
Heel walks
-
Single leg balance
-
Step ups
-
Squats
These exercises are a good starting point for most individuals who do not already have pain. They may need to be altered depending on your ability. To determine the appropriate level, please consult your healthcare provider or doctor of physical therapy.
If you’re already struggling with some pain that just won’t resolve, there are combinations of treatments that might help you out. Give us a call at 480-482-0651 so we can learn more about your issue and how we can help.